LETTER LANGUAGE"Your mammogram shows that your breast tissue is dense. Dense breast tissue is common and is not abnormal. However, dense breast tissue can make it harder to evaluate the results of your mammogram and may also be associated with an increased risk of breast cancer. This information about the results of your mammogram is given to you to raise your awareness and to inform your conversations with your doctor. Together, you can decide which screening options are right for you. A report of your results was sent to your physician."
This year, thousands of Tennessee women will go get a mammogram - just like they do every year.
And while many will see the same results as they did the year before, they may also see an unfamiliar, eyebrow-raising note: "Your mammogram shows that your breast tissue is dense."
The language is drawn from a new state law, which now requires doctors to send these letters out to women who have dense breast tissue.
While it's common, dense tissue can make it more difficult to spot cancer early on in mammograms, and in some cases, it can increase cancer risk, doctors say.
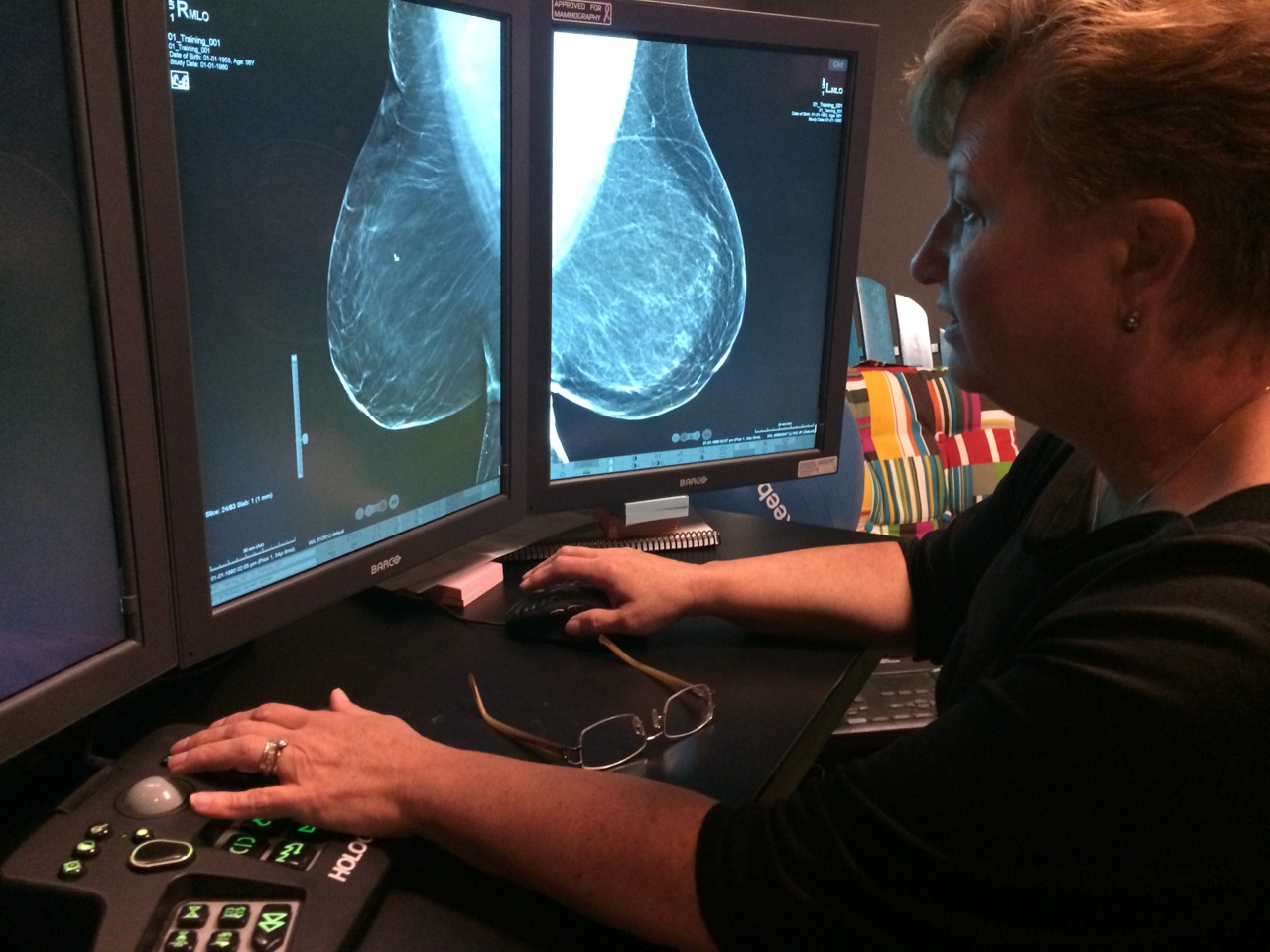
The law is geared toward raising awareness of breast density, explains Dr. Lanett Varnell, a radiologist with the MaryEllen Locher Breast Center, which began sending the letters on Tuesday.
"I think the goal is for women to be aware of what their own situation is. Not to panic, but to become more vigilant," said Varnell.
The law was passed last year and was modeled on laws in 18 other states, pushed by the Connecticut-based nonprofit Are You Dense, Inc. The group advocates for changes to public policy in regard to breast cancer detection.
The understanding of breast density and its relation to cancer detection is nothing new.
Density basically refers to the ratio of connective tissue to fat in the breast. Some breasts are entirely comprised of fat, and some - those on the most dense side of the spectrum - are almost entirely connective tissue. The levels have nothing to do with body fat, and can vary according to age.
On mammogram scans, both the tissue and lumps show up white, meaning higher density can sometimes cloud abnormalities.
Higher density does not necessarily mean women are more in danger of getting breast cancer. But women with especially high breast density may want to talk with their doctor about alternative screenings, like ultrasounds, breast MRIs or a new type of scan called 3D tomosynthesis, which are more effective at reading dense tissue.
By law, the new letters only need to be sent to women whose tissue have 50 percent density. But approximately 40 percent of American women are estimated to fit that category.
"I think it's one more piece of knowledge women have to empower themselves to be in charge of their health and to have an intelligent conversation about what they want their next step to be," said Janet Kramer-Mai, a longtime oncology nurse and breast cancer navigator who is now over the new Breast Cancer Center at Erlanger East.
Kramer-Mai knows the value of that all too well. When she found a lump in her breast in 2001, both a mammogram and a subsequent ultrasound failed to pick up on the cancer that was growing inside of her.
By the time a doctor actually performed a biopsy on the lump several months later, the malignant tumor had grown five centimeters.
Even then an additional mammogram still did not pick up on the lump. The radiologist, crestfallen, showed her how impossible it was to see the tumor amidst her dense tissue.
"I could have totally benefited from this kind of [3D tomosynthesis] screening back then," Kramer-Mai said.
The 3D scans take many scans to capture three-dimensional image of the breast. It was approved in the United States in 2011, and it Chattanooga currently is only available at Memorial - though Erlanger's new breast center plans to have one when it opens later this year.
Local doctors agree that increasing awareness about breast density is important. But they have some concerns about the manner in which it is being pushed. The letters, they say, can be confusing and troubling since they provide little direction about what women are supposed to do next.
"Unfortunately, things that are passed by legislative mandate as opposed to clinical mandate can be a little confusing for patients," said Dr. Trey Carr, director of Medical Imaging at Parkridge Medical Center, which began sending letters earlier this year. "My hope is that it drives some important conversation."
Other critics have said that the law encourages unnecessary screenings, which could lead to biopsies or other procedures that aren't needed.
And health insurance plans typically do not cover these additional screenings, Varnell said, and the legislation doesn't require them to do so.
Memorial screens 40,000 procedures a year, meaning they expect to send out about 20,000 letters within the year.
Erlanger, which began sending the letters out in January, has not seen a major influx in women requesting more tests, said Kramer-Mai.
Carr said that there has been "some confusion" generated by the letters Parkridge has sent.
"Not pandemonium by any means, but women calling with concern," he said.
Contact staff writer Kate Harrison at kharrison@timesfreepress.com or 423-757-6673.